Just now
Aileen MoynaghBBC News NI health reporter

 BBC
BBC
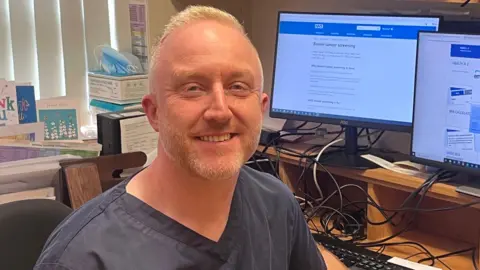
Dr Jonny Dillon wants Northern Ireland's bowel cancer screening programme to be expanded
When Dr Jonny Dillon found out he had bowel cancer at 49 he was shocked - not least because he is a doctor.
He was generally feeling unwell but had no bowel symptoms, yet needed surgery just two days after his 50th birthday.
Now he says he is "very angry" that Northern Ireland's screening programme lags behind the rest of the UK.
The Department of Health (DoH) has said work to expand the programme is ongoing.
Northern Ireland is also the only UK region yet to lower the level at which traces of blood in a home screening test trigger further investigation to detect more bowel cancers early.
Dillon wants the current "excellent screening programme in Northern Ireland" to be expanded.
"I'm calling for the age to be brought down in Northern Ireland from 60 down to 50 and also for the level at which you get further investigations to be reduced in line with England, Scotland, Wales."
"That will pick up cancers or pre cancers at a much earlier stage.
"It will cost money upfront, but that will save money because people will be picked up and it will ultimately save many lives."
The Banbridge GP said his diagnosis was a "huge shock".
As the cancer had not spread, the father of three did not need chemotherapy or radiotherapy and was back working within six months.
"As a GP, I would know that bowel cancer is unusual to have under 50, but we're seeing that the number of people with bowel cancer is increasing."
11.1% of patients diagnosed were under 55.
Why bowel screening is important?

 Getty Images
Getty Images
Screening is currently offered to people aged between 60 and 74 in Northern Ireland
Screening involves a faecal immunochemical test (FIT) to look for blood in a sample of your poo.
It can help detect cancer at an early stage when there are no symptoms and when treatment is more effective.
It can also check for polyps which can develop into cancer.
Polyps can be easily removed, which reduces the risk.
Those eligible for screening who are registered with a GP get a home FIT kit through the post every two years.
Dillon said people in Northern Ireland between 50 and 59 were missing five potential screening opportunities.
In January, NHS England announced it would start using a more sensitive home-screening stool kit, bringing it into line with Scotland and Wales.
In England, Scotland and Wales, the level at which traces of blood in FITs trigger further investigation is 80 micrograms of blood per gram of poo.
In Northern Ireland, it is 120.
A lower level would mean more people being referred for colonoscopies to help diagnose or rule out bowel cancer.
"This isn't screening for a head cold. This is screening for cancer. This is screening for a condition that could result in major surgery or even take your life," Dillon added.
"And if we don't do it, we're resulting in more people losing their life or having to go through major treatment."


Marie McGrath was diagnosed with bowel cancer at the start of 2026
One of Dillon's patients Marie McGrath said "bowel cancer was not on my radar" when she was diagnosed in January, aged 52.
She had a healthy lifestyle and thought it happened to older people.
"Bowel cancer, for me if there were tick boxes, I wouldn't be ticking any boxes.
"It was only in my view because of the professional awareness of my GP, and unfortunately, his own personal experience that I feel I was picked up and picked up well and picked up in time."
Marie went to her GP with an upset tummy that did not settle after returning from holiday last summer.
A colonoscopy found "something of a significant size and of a significant concern".
"I think I went a bit blank, if I'm very honest. She can't really be saying these words to me. This is a tummy bug," she said.
"To have a screening age set at 60, I'm wondering would I have made it to 60 if I hadn't got the GP and the circumstances at the time?
"Had my symptoms maybe been put down to irritable bowel for example, that could have been ongoing for a much longer period of time. What would my chances have been then?
"If much younger people are being affected, why is the threshold so high for us to be diagnosed and diagnosed at an early stage? It just is unfathomable to me."
Genevieve Edwards, Chief Executive of Bowel Cancer UK said Northern Ireland is "falling dangerously behind" on screening.
"If bowel cancer is diagnosed at its earliest stage, more than nine people in 10 will survive it," she said.
"It's treatable, it's curable if it's diagnosed early.
"But we know that one in four people are currently diagnosed in A&E. And that's not the place to find out you've got bowel cancer when your symptoms are advanced, your cancer's advanced, and it's much harder to treat successfully."
She urged the NI Executive to "lower the screening age to 50 without delay".
The DoH said the Northern Ireland Cancer Strategy (2022-32) has committed to reducing the sensitivity levels used in FITs and to lowering the age range in the Bowel Cancer Screening Programme, in line with the UK National Screening Committee recommendation.
It said work to expand the screening programme "is ongoing but must be viewed within the context of wider financial and capacity challenges within the supporting services".
"Where a screening programme expands its eligibility, it is important that the associated infrastructure, including diagnostic capacity, workforce and any treatments that may be required, are aligned," it added.

 2 hours ago
1
2 hours ago
1